Surgical Treatment of Gynaecomastia
Surgical Treatment of Gynaecomastia
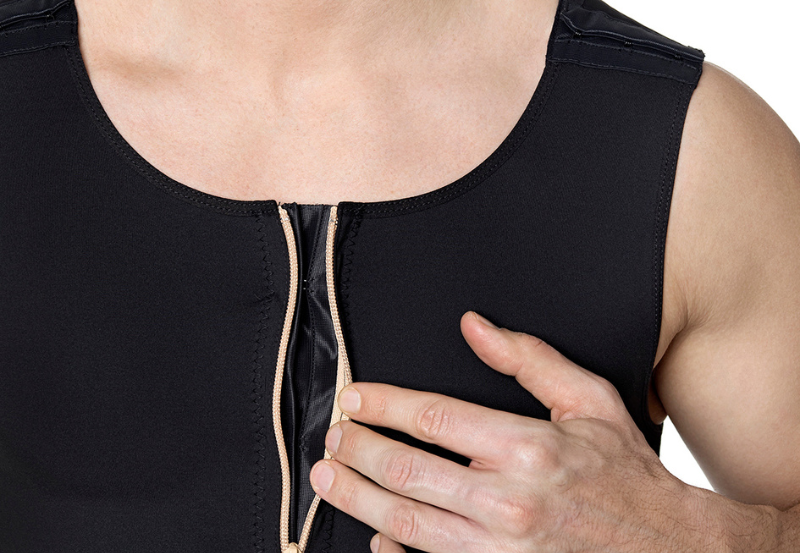
- True or mixed gynecomastia (glandular tissue hypertrophy)
- Lipomastia (excess fatty tissue in the breast)
- Chest asymmetry
- Psychological discomfort related to the appearance of the torso
- No effect after conservative treatment (diet, physical activity)
- Active skin infections on the face or neck
- Uncontrolled chronic diseases (e.g., diabetes, hypertension)
- Blood clotting disorders
- Severe general medical conditions that preclude general anesthesia
- Allergy to anesthetics
- Nierealistyczne oczekiwania co do efektów zabiegu
Preparation for the procedure:
Consultation with a plastic surgeon to determine eligibility, discuss expectations, and plan the procedure
Laboratory tests
Discontinuation of anticoagulants at least 14 days prior to surgery (after consulting a physician)
Avoid alcohol and smoking for at least 14 days before the procedure – for better healing.
Thorough facial skin hygiene on the day of the procedure (no makeup, creams, lotions)
The course of the procedure
The procedure is performed under general anesthesia by a plastic surgery specialist.
The incisions are made in natural skin creases – in front of and behind the ear, sometimes with an additional incision under the chin (in cases of advanced neck sagging).
The SMAS (superficial musculoaponeurotic system) layer is precisely tightened and lifted.
Excess skin is removed and the incision lines are closed with great care to ensure aesthetic scarring.
The whole process usually takes about 2–3 hours.
The patient remains under the care of the clinic – usually 1 day of hospitalization.
Recovery and post-treatment recommendations:
Swelling and bruising are natural and will subside within 2–4 weeks.
It is recommended to sleep with your head elevated for the first few days.
Dressings and sutures cared for according to the doctor's recommendations
Sutures are usually removed after 7–14 days.
Avoid strenuous physical activity and bending over for at least 4–6 weeks.
No sunbathing or solarium use for at least 6 months – SPF 50 protection required
Once fully healed, scar massage and preparations to aid scar maturation may be introduced, as recommended by your doctor.
Follow-up visits: approximately 1 month after the procedure, then after 3, 6, and 12 months
Possible complications and risks:
Hematoma or bleeding requiring drainage
Infection requiring antibiotic therapy
Transient or rarely persistent sensory disturbances in the face or auricle
Hypertrophic or discolored scars – minimized thanks to precise suturing techniques
Asymmetry requiring correction
Prolonged swelling or bruising
Unsatisfactory aesthetic result requiring possible reoperation
Frequently asked questions
Our patients before surgery
No. The procedure is performed under general anesthesia, so the patient does not feel any pain during the operation. After the procedure, there may be a feeling of tension and discomfort, which we alleviate with painkillers.
Most often, it is caused by hormonal disorders, taking certain medications (e.g., steroids), liver disease, or excess body fat. In many patients, the cause remains unknown—this is known as idiopathic gynecomastia.
The scars are thin and run around the areola, which allows them to be concealed as much as possible. In most patients, they become barely visible over time.
For office work, usually after 3–5 days. For physical work, usually after 4 weeks, following a follow-up assessment.
Yes, but only after about 6 weeks and only after a follow-up consultation with your doctor. This applies especially to chest strength training.
We recommend wearing it for a minimum of 4–6 weeks, 24 hours a day with breaks for hygiene. This is a key part of your recovery.
Yes, provided that you maintain a stable body weight and have no hormonal disorders. The effect can be long-term and, in many cases, permanent.
Rarely, but yes—for example, in the event of sudden hormonal changes, resuming medication that disrupts hormone balance, or significant weight gain.
In most cases, yes—to rule out endocrine causes and plan the optimal treatment. The surgeon will determine which tests are necessary during the consultation.
Yes – if the patient is in good general health, gynecomastia can be combined with, for example, liposuction of other areas of the body or nipple correction. The final decision is made by the surgeon.
Do you have any questions?
Get in touch with us
Władysława Syrokomli 46,
51-141 Wrocław
Mon-Fri: 09:00 - 17:00
Saturday - Sunday: closed
Call :+48 666 850 666

